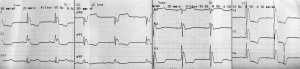
The J-waves of hypothermia
Clinical vignette
A 34-year-old man was found unresponsive on the street, and he was admitted to the emergency department of our Hospital. On arrival, he was still unresponsive with a Glasgow Coma Scale of 9. A cold skin during physical examination was evident. His vital signs were blood pressure 100/65 mmHg, heart rate 46 bpm, core temperature 32 °C and respiratory rate 12/min. No further information was available about his medical history. Electrocardiogram (ECG) on admission revealed sinus bradycardia with prominent J-waves and prolonged QT interval in nearly every lead (Figure 1). Intravenous fluids were immediately administered and the patient underwent active and passive rewarming in the Intensive Care Unit along with continuous rhythm monitoring. The patient’s cognitive status improved rapidly during the next hours following rewarming. The ECG demonstrated progressive normalization of the QT interval, while the J-waves amplitude was gradually decreased in an inverse relation manner to the core temperature. When his core temperature reached normal range, the ECG became unremarkable. He was subsequently transferred to the medical floor and after a few days he was discharged fully recovered.
ECG description and discussion
The ECG at the time of admission to the emergency room (Figure 1) revealed sinus bradycardia. The QRS axis was normal. The QRS duration was 100 msec, the PR interval was slightly prolonged (250 msec), and the QTc interval (Fridericia’s equation) was markedly prolonged (590 msec). Prominent J-waves were present in nearly every lead along with diffuse ST-segment and T-wave abnormalities mostly discordant to the QRS vector.
Hypothermia is known to produce several ECG changes primarily due to action potential lengthening, myocardial conduction slowing and prolongation of depolarization (1). Common findings during hypothermia are sinus bradycardia, junctional rhythm, atrial fibrillation, prolonged PR and QT intervals, prominent J-waves, and T-wave changes. Profound hypothermia predisposes to ventricular fibrillation (VF) (1).
The J-waves of hypothermia is a specific morphologic pattern of a deflection with a dome or hump morphology in the same direction as R wave, occurring in the R-ST junction. J-wave was named “Osborn wave” after Osborn’s landmark article, concerning the effect of induced hypothermia on the respiratory and cardiac function of dogs and the development of this deflection on the surface ECG, which he called “current of injury” (2). Transmural differences in the early phases of the action potential (phases 1 and 2) are responsible for inscription of the J-wave. The seminal work from C. Antzelevitch’s group have demonstrated that prominent Ito-mediated action potential notch in ventricular epicardium but not endocardium produces a transmural voltage gradient in the early phase of ventricular repolarization that manifests as a J-wave on the ECG (3). Accentuation of the action potential notch and loss of the dome are due to an outward shift of currents secondary to either a decrease in inward currents (INa and ICa) or an increase in outward potassium currents (3,4). Loss of the action potential dome is heterogeneous and results in marked abbreviation of the action potential at some sites but not at others, and may give rise to ventricular arrhythmias (phase 2 reentry) (3,4).
The J-waves have been associated with many inherited or acquired conditions, such as the Brugada syndrome (BrS), early repolarization syndrome (ERS), hypercalcemia, myocardial ischemia, and subarachnoid hemorrhage (4). Intrinsic connection exists in the molecular basis of BrS and ERS that have been grouped under the umbrella of J-wave syndromes. J-wave syndromes have been associated with an increased risk of VF and/or sudden cardiac death (4).
Points to ponder
Electrocardiographic manifestations of hypothermia may assist in timely diagnosis and management of hypothermic patients. Even though prominent J-waves are the hallmark of hypothermic patient’s ECG, they are not pathognomonic, as they have been associated with other inherited or acquired conditions, many of which are highly arrhythmogenic.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Mallet ML. Pathophysiology of accidental hypothermia. QJM 2002;95:775-85. [Crossref] [PubMed]
- Osborn JJ. Experimental hypothermia; respiratory and blood pH changes in relation to cardiac function. Am J Physiol 1953;175:389-98. [Crossref] [PubMed]
- Yan GX, Antzelevitch C. Cellular basis for the electrocardiographic J wave. Circulation 1996;93:372-9. [Crossref] [PubMed]
- Antzelevitch C, Yan GX. J wave syndromes. Heart Rhythm 2010;7:549-58. [Crossref] [PubMed]