
The role of the stapled interlobar fissure position for intraoperative detection and postoperative diagnosis of middle lobe torsion after right upper lobectomy
Highlight box
Key findings
• On postoperative computed tomography (CT) scans, the stapled interlobar fissure (SIF) position was on the interlobar side in 24 (96.0%) of 25 patients with abnormal findings in the middle lobe (ML), and on the mediastinal side in 224 (91.1%) of 246 patients without abnormalities (P<0.001).
• At the end of the surgery, the SIF position was on the interlobar side in 10 (90.9%) of 11 patients with abnormal findings in the ML, and on the mediastinal side in 53 (86.9%) of 61 patients without abnormalities (P<0.001).
What is known and what is new?
• Characteristic CT and bronchoscopy findings, such as atelectasis and rotation of the bronchus and pulmonary vessels, are useful for the diagnosis of ML torsion following right upper lobectomy (RUL).
• Based on the results of this study, by focusing on the SIF position of the ML after RUL, torsion of the lung could be easily determined, regardless of whether treatment is required.
What is the implication, and what should change now?
• The SIF position observed at the end of the surgery and on postoperative CT scans was significantly associated with postoperative ML abnormalities.
• Monitoring the SIF position may aid in intraoperative detection and postoperative diagnosis of ML torsion after RUL.
Introduction
Lung torsion is caused by the lung twisting around the hilum, leading to congestion, ischemia, and atelectasis; it has a high mortality rate of 22% (1). This is an important condition for thoracic surgeons to recognize. Although the incidence rate is reported to be 0.089–0.4% (2), 30% of thoracic surgeons in the United Kingdom encounter lung torsion in clinical practice, suggesting that many thoracic surgeons may experience it (3). The causes are reported to be idiopathic (4), pleural effusion (5), and post-lung transplantation (6), but most cases occur after lung resection. The most common occurrence after lung resection is middle lobe (ML) torsion following right upper lobectomy (RUL) (2). Characteristic computed tomography (CT) and bronchoscopy findings are useful for the diagnosis (7).
Recently, it has been reported that stapled interlobar fissure (SIF) position is related to the diagnosis of ML torsion (8,9). Koike et al. reported the SIF position of the ML on postoperative CT in 82 cases of RUL (8). In this report, if the SIF position was on the interlobar side, the ML was considered to be rotated 120-degree counterclockwise. They reported that ML rotation was present in 11% of cases and was associated with serious postoperative complications such as atelectasis and pneumonia. Surgical videos of cases with rotation were reviewed, suggesting that careful positioning of the ML at the end of surgery may prevent ML rotation. Limitations of this study include the relatively small cohort size, the single-center study, and the fact that surgical videos of patients with no ML rotation were not reviewed.
In this study, we aimed to evaluate the usefulness of the SIF position for intraoperative detection and postoperative early diagnosis of ML torsion by retrospectively reviewing a relatively large number of cases of RUL performed at two institutions. We present this article in accordance with the STROBE reporting checklist (available at https://jtd.amegroups.com/article/view/10.21037/jtd-2024-1960/rc).
Methods
Study design
In this retrospective study, 334 patients who underwent RUL at Hokkaido University Hospital or Obihiro Kosei General Hospital between January 2015 and May 2022, regardless of the disease type, were initially reviewed. Finally, 271 patients were included in the study because they had an interlobar fissure between the upper lobe and ML divided using a surgical stapler, and had undergone at least one chest CT scan postoperatively, including CT scans taken at the onset of post-operative symptoms or at follow-up for lung cancer or other diseases, regardless of when it was taken (Figure 1). The 271 patients comprised 103 males and 168 females with a median age of 71 years (range, 41–87 years). Diagnoses included 259 primary lung cancers, five metastatic lung tumors and seven others.

We evaluated the correlation between the SIF position and the abnormal findings in the ML on postoperative CT scans. Additionally, we reviewed the surgical videos of the patients to confirm the SIF position at the end of the surgery and evaluated its correlation with postoperative abnormal findings in the ML. Note that only CT findings taken in the first postoperative period were collected in this study, and no subsequent CT findings were collected.
This study underwent centralized review and was approved by the Institutional Review Board of Hokkaido University Hospital (approval number: 024-0062) because Obihiro Kosei General Hospital was treated as an institution that solely provides existing information. Obihiro Kosei General Hospital was informed and agreed with the study. The study was conducted in accordance with the Helsinki Declaration (revised in 2013). Individual consent for this retrospective analysis was waived.
Operative procedure and postoperative management
In both hospitals, video-assisted thoracic surgery (VATS) was the standard approach for RUL. The number of incisions varied according to each patient. Open thoracotomy was mainly performed under the following conditions: when the tumor was large, or when vascular or bronchial reconstruction was required. Robot-assisted thoracic surgery (RATS) was introduced as an approach starting in 2020.
The main procedures were: the upper lobe bronchus, upper lobe branches of the superior pulmonary vein, and superior trunk of the pulmonary artery were divided using a surgical stapler. The other branches of the pulmonary artery were divided after ligation or stapling using a surgical stapler. The interlobar fissures between the upper lobe and ML and those between the upper and lower lobes were divided using electrocautery or an energy device if the fissures were not fused. If the fissures were fused, they were divided using a surgical stapler. Although the order of division varied among cases, the bronchus was generally divided last. The fissureless technique was used in cases of severely fused interlobar fissures. In this technique, the vessels and bronchus are divided first, followed by the simultaneous division of the upper-middle and upper-lower fissures (10). After the leakage test and drain placement, the procedure was completed by visually confirming inflation of the remaining lobes. Unless lung torsion is detected intraoperatively, no procedures are taken to prevent it.
Postoperatively, the drain was removed when there was no leakage and the pleural effusion was less than 300 mL. Chest radiographs were obtained daily until the day after the drain removal. If any symptoms were reported, chest CT or bronchoscopy was performed as needed. For malignant diseases, CT scans were conducted three to 6 months postoperatively to check for recurrence. The use of contrast agents was determined by the attending physician.
Data collection and definitions
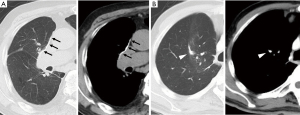
Clinical and surgical data were collected from medical records and databases of each hospital. The initial postoperative CT images were retrospectively reviewed. The SIF position of the ML was assessed to determine whether it was on the mediastinal or interlobar side (Figure 2). There were in which the SIF position was continuous from the mediastinal to interlobar side, in which case it was considered to be on the mediastinal side. Additionally, abnormal findings in the ML were assessed for complete atelectasis, partial atelectasis, or rotation of the bronchus and pulmonary vessels on chest CT images only, which were defined as findings of ML torsion in the present study (Figure 3). The ML bronchus was traced distally, and bronchial rotation was defined if B4 was directed towards the typical location of S5, and B5 was directed towards the typical location of S4.

Surgical videos were reviewed to verify the SIF position of the ML at the end of the surgery. The SIF position at the end of the surgery was confirmed in 72 patients. We assessed whether the SIF of the ML was directed towards the mediastinal side or the interlobar surface of the lower lobe at the end of the surgery (Figure 4).

Statistical analysis
Univariate analyses of background factors were performed using the Mann-Whitney U test for quantitative variables or Fisher’s exact test for qualitative variables. Sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), positive likelihood ratio (PLR), and negative likelihood ratio (NLR) were used to determine diagnostic accuracy. Statistical analyses were performed using JMP Pro17 (SAS Institute Inc., Cary, NC, USA). A P value of less than 0.05 was considered significant.
Results
Patient characteristics are shown in Table 1. Abnormal findings in the ML on postoperative CT scans were observed in 25 patients (9.2%). Eleven patients had atelectasis and 14 had vascular and bronchial rotation. Two patients required re-operation because of abnormal findings in the ML.
Table 1
| Variables | Abnormal findings in the ML | P value | |
|---|---|---|---|
| + (n=25) | − (n=246) | ||
| Age (years) | 72 [53–87] | 70 [41–86] | 0.29† |
| Sex | 0.83‡ | ||
| Male | 10 (40.0) | 93 (37.8) | |
| Female | 15 (60.0) | 153 (62.2) | |
| Diagnosis | 0.53‡ | ||
| Primary lung cancer | 25 (100.0) | 234 (95.1) | |
| Metastatic lung tumor | 0 (0.0) | 5 (2.0) | |
| Others | 0 (0.0) | 7 (2.8) | |
| Body mass index (kg/m2) | 22.0 [17.1–29.1] | 22.6 [14.0–37.4] | 0.48† |
| %VC | 117.0 [89.3–144.7] | 106.8 [59.3–195.7] | 0.056† |
| FEV1% | 71.9 [46.9–144.1] | 73.8 [39.9–107.5] | 0.24† |
| Surgical approach | 0.65‡ | ||
| VATS | 19 (76.0) | 203 (82.5) | |
| RATS | 4 (16.0) | 25 (10.2) | |
| Open thoracotomy | 2 (8.0) | 18 (7.3) | |
| Mediastinal lymph node dissection | 23 (92.0) | 229 (93.1) | 0.69‡ |
| Operative time (minutes) | 210 [72–454] | 222 [112–566] | 0.70† |
| Division of the interlobar fissure between the upper and lower lobe | 0.15‡ | ||
| Surgical stapler | 19 (76.0) | 151 (61.4) | |
| Electrocautery/energy device | 6 (24.0) | 95 (38.6) | |
| Reoperation | 2 (0.7) | 0 (0.0) | NA |
Data are presented as median [range] or n (%). †, continuous variables were compared using the Mann-Whitney U test; ‡, frequencies were compared using Fisher’s exact test for categorical variables. +, patients with abnormal findings; −, patients without abnormal findings. FEV1%, forced expiratory volume in 1 second; ML, middle lobe; NA, not available; RATS, robot-assisted thoracic surgery; VATS, video-assisted thoracic surgery; %VC, percent predicted vital capacity.
The SIF position on postoperative CT scans
Among the 25 patients with abnormal findings in the ML on postoperative CT scans, the SIF position was on the interlobar side in 24 patients (96.0%) and on the mediastinal side in 1 patient (4.0%) (Table 2). One of the patients with the SIF position on the interlobar side, with symptoms and abnormal laboratory findings, underwent re-operation due to ML torsion. The one patient with the SIF position on the mediastinal side underwent re-operation because of complete ML atelectasis; however, torsion was not observed and was considered to be due to ML bronchial kinking. The remaining 23 patients were not treated because they had no symptoms and no abnormal laboratory findings. Bronchoscopy was only performed in two cases where reoperation was performed because of symptoms and suspected torsion.
Table 2
| SIF position | Abnormal findings in the ML | P value | |
|---|---|---|---|
| + (n=25) | − (n=246) | ||
| Mediastinal | 1 (4.0) | 224 (91.1) | <0.001† |
| Interlobar | 24 (96.0) | 22 (8.9) | |
Data are presented as n (%). †, frequencies were compared using Fisher’s exact test for categorical variables. +, patients with abnormal findings; −, patients without abnormal findings. CT, computed tomography; ML, middle lobe; SIF, stapled interlobar fissure.
In 246 patients without abnormal findings in the ML on postoperative CT scans, the SIF position was on the interlobar side in 19 patients (7.7%), on the mediastinal side in 224 patients (91.1%), and continuous from the mediastinal to interlobar side in 3 patients (1.2%).
The SIF position on postoperative CT scans was associated with abnormal findings in the ML (P<0.001). For the diagnosis of abnormal findings of the ML based on the SIF position on postoperative CT scans, the sensitivity and specificity were 96.0% and 91.1%, respectively. The PLR was 10.735 [95% confidence interval (CI): 7.148–16.122], and the NLR was 0.044 (95% CI: 0.006–0.300). The PPV was 52.2% (95% CI: 36.9–67.1%), and the NPV was 99.6% (95% CI: 97.5–100%).
A similar analysis was performed by focusing specifically on atelectasis among the abnormal findings in the ML (Table 3). In 11 patients of ML atelectasis on postoperative CT scans, the SIF was positioned on the interlobar side in 10 patients (90.9%) and on the mediastinal side in 1 patient (9.1%). In 260 patients without ML atelectasis on postoperative CT scans, the SIF was positioned on the interlobar side in 36 patients (13.8%) and on the mediastinal side in 224 patients (86.2%).
Table 3
| SIF position | ML atelectasis | P value | |
|---|---|---|---|
| + (n=11) | − (n=260) | ||
| Mediastinal | 1 (9.1) | 224 (86.2) | <0.001† |
| Interlobar | 10 (90.9) | 36 (13.8) | |
Data are presented as n (%). †, frequencies were compared using Fisher’s exact test for categorical variables. +, patients with ML atelectasis; −, patients without ML atelectasis. CT, computed tomography; ML, middle lobe; SIF, stapled interlobar fissure.
The SIF position on postoperative CT scans was associated with ML atelectasis (P<0.001). For the diagnosis of ML atelectasis based on the SIF position on postoperative CT scans, the sensitivity and specificity were 90.9% and 86.2%, respectively. The PLR was 6.566 (95% CI: 4.598–9.375), and the NLR was 0.106 (95% CI: 0.016–0.684). The PPV was 21.7% (95% CI: 10.9–36.4%), and the NPV was 99.6% (95% CI: 97.5–100%).
The SIF position at the end of the surgery
We examined 72 patients where the SIF position at the end of the surgery was confirmed in the surgical video (Table 4). In 11 patients with abnormal findings in the ML on postoperative CT scans, the SIF position at the end of the surgery was on the interlobar side in 10 patients (90.9%) and on the mediastinal side in 1 patient (9.1%). In 61 patients without abnormal findings in the ML on postoperative CT scans, the SIF position at the end of the surgery was on the interlobar side in 8 patients (13.1%) and on the mediastinal side in 53 patients (86.9%).
Table 4
| SIF position | Abnormal findings in the ML | P value | |
|---|---|---|---|
| + (n=11) | − (n=61) | ||
| Mediastinal | 1 (9.1) | 53 (86.9) | <0.001† |
| Interlobar | 10 (90.9) | 8 (13.1) | |
Data are presented as n (%). †, frequencies were compared using Fisher’s exact test for categorical variables. +, patients with abnormal findings; −, patients without abnormal findings. ML, middle lobe; SIF, stapled interlobar fissure.
The SIF position at the end of the surgery was associated with abnormal findings in the ML (P<0.001). For the prediction of abnormal findings in the ML based on the SIF position at the end of the surgery, the sensitivity and specificity were 90.9% and 86.9%, respectively. The PLR was 6.932 (95% CI: 3.539–13.579), and the NLR was 0.105 (95% CI: 0.016–0.680). The PPV was 55.6% (95% CI: 30.8–78.5%), and the NPV was 98.1% (95% CI: 90.1–100%).
A similar analysis was performed focusing specifically on atelectasis among the abnormal findings in the ML (Table 5). In four patients with ML atelectasis on postoperative CT scans, the SIF position at the end of the surgery was on the interlobar side in 3 patients (75.0%) and on the mediastinal side in 1 patient (25.0%). In 68 patients without ML atelectasis on postoperative CT scans, the SIF position at the end of the surgery was on the interlobar side in 15 patients (22.1%) and on the mediastinal side in 53 patients (77.9%).
Table 5
| SIF position | ML atelectasis | P value | |
|---|---|---|---|
| + (n=4) | − (n=68) | ||
| Mediastinal | 1 (25.0) | 53 (77.9) | 0.045† |
| Interlobar | 3 (75.0) | 15 (22.1) | |
Data are presented as n (%). †, frequencies were compared using Fisher’s exact test for categorical variables. +, patients with ML atelectasis; −, patients without ML atelectasis. SIF, stapled interlobar fissure.
The SIF position at the end of the surgery was associated with ML atelectasis (P=0.045). For the prediction of ML atelectasis based on the SIF position at the end of the surgery, the sensitivity and specificity were 75.0% and 77.9%, respectively. The PLR was 3.400 (95% CI: 1.653–6.992), and the NLR was 0.321 (95% CI: 0.058–1.759). The PPV was 16.7% (95% CI: 3.6–41.4%), and the NPV was 98.1% (95% CI: 90.1–100%).
Discussion
In this study, we examined the relationship between the SIF position and postoperative ML abnormalities in patients who underwent RUL. The SIF position on postoperative CT scans was strongly associated with postoperative ML abnormalities. Additionally, the SIF position at the end of the surgery was strongly associated with postoperative ML abnormalities. Since ML torsion involves atelectasis and rotation of the blood vessels and bronchus, which were defined as abnormal findings in this study, the SIF position at the end of the surgery and on postoperative CT scans could be useful for intraoperative detection and postoperative early diagnosis of ML torsion. If the SIF is on the interlobar side on CT scans, it suggests that ML torsion can be diagnosed by considering the symptoms and clinical findings without bronchoscopy. If the SIF is on the interlobar side at the end of the surgery, it suggests a higher likelihood of postoperative ML torsion. Although lung torsion can also occur due to other factors, such as pneumothorax or pleural effusion, at least torsion that has already developed during surgery could be detected early.
An abnormal position of the SIF indicates that the ML is at least rotated. In this study, 24 (96%) of 25 patients with abnormal findings in the ML on postoperative CT scans showed an abnormal SIF position. Among these, one patient was symptomatic and was diagnosed with torsion, leading to re-operation. The remaining 23 patients were asymptomatic and did not present any clinical problems. Therefore, even if the ML is twisted, this is likely not to be a clinical problem in many cases. Indeed, cases of ML atelectasis are occasionally experienced in cases that improve spontaneously with untreated follow-up. ML torsion becomes problematic when complete obstruction of the bronchus and pulmonary vessels occurs. In such cases, it can lead to atelectasis, ischemia, congestion, and necrosis of the lung parenchyma, resulting in respiratory failure and acute respiratory distress syndrome (6). Even partial 90-degree torsion can cause these problems (2,11). As progression to such a critical state can be fatal, it is important to prevent or diagnose torsion early, even if it often does not cause clinical problems. Additionally, it is not necessary to perform CT scans in all cases after RUL, but CT scans should be actively considered if there are any clinical findings.
In this study, among the 46 patients where the SIF was on the interlobar side on postoperative CT scans, 10 patients (21.7%) showed ML atelectasis. One patient was diagnosed with torsion and underwent detorsion. Two patients showed an improvement in atelectasis several months later. Additionally, among the 225 patients in which the SIF was on the mediastinal side, 1 patient (0.4%) showed ML atelectasis. The patient underwent re-operation to confirm the absence of torsion and was diagnosed with ML bronchial kinking. Although only one patient required therapeutic intervention, ML atelectasis was clearly more common in patients where the SIF was on the interlobar side. In a similar study by Koike et al., the frequency of atelectasis was higher in patients with ML rotation (8). This may be due to bronchial kinking in addition to bronchial twisting. Bronchial kinking occurs when, after upper lobectomy, the diaphragm elevates and the remaining middle and lower lobes shift cranially, causing “sigmoidal distortion” of the bronchus (2). Ueda et al. reported that bronchial kinking, defined as airway obstruction or narrowing of more than 80% of the lumen, was observed in 34% of patients after RUL (12). The ML bronchus is prone to narrowing naturally over time after RUL, and the additional twisting of the ML bronchus may have contributed to the increased incidence of atelectasis.
Generally, thoracic surgeons confirm that the remaining lung is inflated at the end of the surgery. If the ML was inflated, it was assumed that torsion did not occur. However, even if torsion is present, as long as the bronchus is not completely obstructed, the ML can be easily inflated with positive-pressure ventilation. Therefore, it would be dangerous to conclude that there is no torsion simply because the ML inflates. Our study results confirmed that SIF of the ML facing the mediastinal surface could help detect torsion. In fact, after the analysis of this study, we encountered a patient in which although the ML was well inflated at the end of the surgery, we detected a 270-degree clockwise torsion due to the abnormal SIF position. Torsion can occur clockwise or counterclockwise; however, in the patient of 360-degree torsion, the SIF may appear in a normal position (13). However, a 360-degree torsion is expected to be accompanied by bronchial obstruction. Therefore, it is important to confirm both inflation of the ML and correct SIF positioning at the end of the surgery to detect torsion that has already developed during surgery.
Risk factors for torsion include atelectasis, a long bronchovascular pedicle, complete lobulation, pneumothorax, pleural effusion, and division of the inferior pulmonary ligament (14). Preventive procedures may be performed before chest closure if these risks are identified during surgery. Many thoracic surgeons would suture the middle to lower lobe (13). Other preventive procedures reported include using an absorptive sheet and fibrin glue (15), TachoSil® (16), and a pleural flap (17). These preventive procedures have not been proven through prospective studies but are often employed based on empirical experience. In this study, all 14 patients who underwent fissureless lobectomy had SIF on the mediastinal surface on postoperative CT scans. Although this technique is generally performed in patients of poor lobulation, the continuous stapled line from the middle to lower lobe may help prevent excessive displacement or torsion of the ML.
This study had several limitations. First, it was a retrospective study. Secondly, the degree of lobulation was not assessed. Third, details of the division between the upper lobe and ML were not assessed. For example, when a tumor is located near the interlobar area of S3, the interlobar fissure may be divided into the ML. This could deform the ML, potentially reducing the accuracy of the relationship between the SIF position and the degree of ML torsion. Forth, this study had a small number of cases, especially those in which surgical videos could be analyzed.
Conclusions
The SIF position at the end of the surgery and on postoperative CT scans was associated with postoperative ML atelectasis and rotation of the blood vessels and bronchus. Because ML torsion involves atelectasis and rotation of the blood vessels and bronchus, the SIF position may be useful for early diagnosis of ML torsion and even for early detection of torsion that has already developed during surgery.
Acknowledgments
We would like to thank Editage (https://www.editage.com/) for English language editing.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at https://jtd.amegroups.com/article/view/10.21037/jtd-2024-1960/rc
Data Sharing Statement: Available at https://jtd.amegroups.com/article/view/10.21037/jtd-2024-1960/dss
Peer Review File: Available at https://jtd.amegroups.com/article/view/10.21037/jtd-2024-1960/prf
Funding: None.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jtd.amegroups.com/article/view/10.21037/jtd-2024-1960/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). This study underwent centralized review and was approved by the Institutional Review Board of Hokkaido University Hospital (approval number: 024-0062) because Obihiro Kosei General Hospital was treated as an institution that solely provides existing information. Obihiro Kosei General Hospital was informed and agreed with the study. Individual consent for this retrospective analysis was waived.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Kanaan S, Boswell WD, Hagen JA. Clinical and radiographic signs lead to early detection of lobar torsion and subsequent successful intervention. J Thorac Cardiovasc Surg 2006;132:720-1. [Crossref] [PubMed]
- Dai J, Xie D, Wang H, et al. Predictors of survival in lung torsion: A systematic review and pooled analysis. J Thorac Cardiovasc Surg 2016;152:737-745.e3. [Crossref] [PubMed]
- Wong PS, Goldstraw P. Pulmonary torsion: a questionnaire survey and a survey of the literature. Ann Thorac Surg 1992;54:286-8. [Crossref] [PubMed]
- Ternes T, Trump M, de Christenson MR, et al. Spontaneous middle-lobe torsion. Radiol Case Rep 2013;8:812. [Crossref] [PubMed]
- Donato BB, Sewell M, Al Harakeh H, et al. Spontaneous middle lobe torsion: An institutional case series. JTCVS Tech 2023;20:176-81. [Crossref] [PubMed]
- Cox CS, Decker SJ, Rolfe M, et al. Middle Lobe Torsion after Unilateral Lung Transplant. J Radiol Case Rep 2016;10:15-21. [Crossref] [PubMed]
- Tamizuddin F, Ocal S, Toussie D, et al. Differentiating Imaging Features of Post-lobectomy Right Middle Lobe Torsion. J Thorac Imaging 2023; Epub ahead of print. [Crossref] [PubMed]
- Koike S, Eguchi T, Matsuoka S, et al. Impact of counterclockwise rotation of the right middle lobe following right upper lobectomy. Interact Cardiovasc Thorac Surg 2022;34:1062-70. [Crossref] [PubMed]
- Yanagihara T, Ichimura H, Kobayashi K, et al. Computed tomography detection of stapled interlobar fissure facilitates diagnosing postoperative lobar torsion: A case report. Int J Surg Case Rep 2017;41:86-8. [Crossref] [PubMed]
- Temes RT, Willms CD, Endara SA, et al. Fissureless lobectomy. Ann Thorac Surg 1998;65:282-4. [Crossref] [PubMed]
- Taira N, Kawasaki H, Takahara S, et al. Lingular segment torsion following a left upper division segmentectomy. Int J Surg Case Rep 2017;39:77-9. [Crossref] [PubMed]
- Ueda K, Tanaka T, Hayashi M, et al. Clinical ramifications of bronchial kink after upper lobectomy. Ann Thorac Surg 2012;93:259-65. [Crossref] [PubMed]
- Sticco CC, Andaz S, Fox S. Middle lobe torsion after right upper lobectomy: a report of video-assisted thoracoscopic management. J Thorac Cardiovasc Surg 2007;134:1090-1. [Crossref] [PubMed]
- Felson B. Lung torsion: radiographic findings in nine cases. Radiology 1987;162:631-8. [Crossref] [PubMed]
- Matsumiya H, Kuroda K, Mori M, et al. Dislocation of a middle lobe torsion-preventing bridging structure with an absorptive sheet and fibrin glue: a case report. Surg Case Rep 2022;8:207. [Crossref] [PubMed]
- Fiorelli A, Scaramuzzi R, Costanzo S, et al. Interlobar fixation using TachoSil(®): a novel technique. Transl Lung Cancer Res 2015;4:605-9. [PubMed]
- Kutlu CA, Olgac G. Pleural flap to prevent lobar torsion: A novel technique. Eur J Cardiothorac Surg 2006;30:943-4. [Crossref] [PubMed]


